Last Updated on August 1, 2024 by MASSAGE Magazine

Any discussion of shoulder pathologies must start with a solid understanding of the anatomical and biomechanical challenges in this area.
Shoulder pain is common because the shoulder is complex. The main joint, the glenohumeral joint, has a wide range of motion but is prone to issues. The shoulder includes the scapula, humerus, and clavicle, with many muscles and ligaments controlling movement. Key areas like the subacromial region can get compressed, causing impingement syndrome. Conditions like frozen shoulder and weak muscles can also cause problems. Massage therapy helps by improving muscle function and reducing nerve pressure, but some issues, like a hooked acromion, might need surgery. Understanding these factors helps massage therapists provide better treatments.
Architecture and Mechanics
Any discussion of shoulder pathologies must start with a solid understanding of the anatomical and biomechanical challenges in this area. The scapula and humerus are the two main bones of the shoulder complex, although the clavicle is another essential bone in the shoulder girdle.
The glenohumeral joint is what we generally refer to as the shoulder joint and it is the articulation between the humerus and scapula. Soft tissues attaching to the shoulder bones are crucial in governing the complex movements of the shoulder as there are close to 20 muscles attaching to the scapula. Ligaments that bind the bones of the shoulder girdle also play a key role in numerous pathologies.
One area of the shoulder, the subacromial region, is particularly important in a number of soft-tissue pathologies. The subacromial region lies beneath the coracoacromial arch. This arch is formed by two bony projections, the coracoid process and acromion process of the scapula. The coracoacromial ligament spans between these two bony prominences to form the arch.
Soft tissues such as the supraspinatus tendon, subacromial bursa, joint capsule, coracohumeral ligament, and biceps brachii tendon all pass underneath the coracoacromial arch (Fig. 1). During shoulder flexion or abduction, any of these soft tissues can be compressed under the coracoacromial arch; repeated compression can cause fraying, irritation and inflammation. Compression of the soft tissues underneath the coracoacromial arch is referred to as shoulder impingement syndrome.
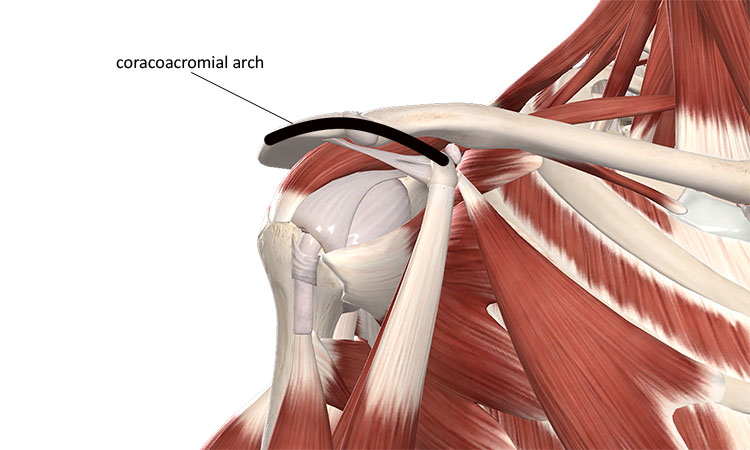
Image courtesy of Complete Anatomy
Keep in mind we frequently hear the term impingement in relation to nerve compression pathologies, but there are no nerves compressed in shoulder impingement syndrome.
The most common tissue injured under the coracoacromial arch is the supraspinatus tendon. A diagnosis of rotator cuff tears usually implicates the supraspinatus, although the subscapularis can also be susceptible to some minor degree of compression under the arch. Rotator cuff tears are common and affect roughly 40% of the population over 60 years of age. We’ll look at some other key issues around rotator cuff tears below.
Mechanics’ Contribution to Shoulder Pathologies
In addition to structure, it is crucial to understand how shoulder mechanics contribute to various complaints. For example, shoulder abduction involves coordinated movement between the scapula and humerus. Full abduction requires upward rotation of the scapula along with glenohumeral abduction in a specific ratio.
During shoulder abduction, for every two degrees of abduction at the glenohumeral joint there is one degree of upward rotation at the scapulothoracic articulation. This coordinated movement is referred to as the scapulothoracic rhythm. Various conditions, such as adhesive capsulitis (frozen shoulder), cause a significant alteration of the scapulohumeral rhythm.
In adhesive capsulitis there is an impairment to full glenohumeral movement, and abduction of the upper extremity may emphasize the client’s upward rotation of the scapula. When this occurs, clients are unable to fully abduct the glenohumeral joint and will laterally flex the torso to the opposite side when attempting to abduct the upper extremity. For example, if a client has adhesive capsulitis on the right side, they will often bend to the left in an attempt to lift their right arm farther out to the side.
There is another fascinating aspect to this issue of the coordinated upward rotation of the scapula and glenohumeral abduction. In some cases it is scapular rotation that is limited instead of glenohumeral abduction. This can occur as a result of weakness in the serratus anterior muscle. Serratus anterior weakness is also apparent when the client is prone on the treatment table because it often shows up as scapular “winging.”
The most common cause of serratus anterior weakness is compression of the long thoracic nerve, which lies close to the brachial plexus in the neck. This nerve is often compressed by heavy straps worn across the shoulders, such as backpacks, handbags, or other types of equipment bags. The long thoracic nerve is primarily a motor nerve and the majority of its fibers supply innervation to the serratus anterior.
Long thoracic nerve compression causes serratus anterior weakness. When the serratus anterior is weak, the client is not able to fully move the scapula into upward rotation during upper extremity abduction. When the scapula doesn’t fully rotate upward during abduction, the greater tubercle of the humerus pinches soft tissues against the underside of the acromion (shoulder impingement). This pattern reminds us that it is important to look at a variety of factors that can contribute to shoulder impingement; sometimes the cause may be a bit more elusive than is immediately apparent.
Massage Approaches for Shoulder Pathologies
In the examples above with adhesive capsulitis, shoulder impingement, and rotator cuff damage, there are clear aspects of soft-tissue pathology that can be addressed with a variety of massage approaches. However, sometimes there are aspects of shoulder structure that won’t be as responsive to massage treatment. A good example is the hooked acromion.
The acromion process can have different shapes, and its shape may change as a person ages. The most common is the Type 1 or flat acromion, in which the underside of the acromion is relatively flat. The Type 2, or curved acromion, has a curved shape which is concave on the inferior side of the acromion. It is the Type 3 or “hooked” acromion that warrants special attention in many subacromial impingement problems (Fig. 2).

Image courtesy of Academy of Clinical Massage
Various structures in the body change shape as we age. The acromion’s shape changes in reaction to mechanical and physiological forces acting on the structures that attach to it. The coracoacromial ligament, which we discussed earlier, spans between the coracoid and acromion processes of the scapula.
Tensile forces transmitted through the coracoacromial ligament pull on its attachment site at the acromion process. The body often develops calcification in regions where the bone is stressed as it perceives a bony injury. Calcification occurs at this attachment site in reaction to the constant pulling of the soft tissues at the attachment site.
After some time the calcification builds up into the hooked acromion shape. The hooked acromion decreases the space between the acromion process and the humerus so all the soft tissues in the subacromial space are more easily pinched with a hooked acromion. Surgery is usually the preferred treatment for a hooked acromion, as a surgeon can shave off the underside of the hooked bone and make more space so the soft tissues aren’t as vulnerable to compression.
Treatment Considerations for Shoulder Pathologies
Conditions such as shoulder impingement can be challenging to treat with massage. Because the supraspinatus lies mostly under the acromion process, it is difficult to access with our treatments. We can get to the most distal aspects of the supraspinatus tendon near its attachment site, but the distal tendon is still deep to the deltoid muscle, which we must work through.
Even though much of the supraspinatus tendon is not easily accessible, working all of the muscles of the shoulder girdle can still be helpful in addressing shoulder complaints. As we noted earlier, over 20 muscles attach to the scapula alone, so the muscular components of the shoulder girdle play a major role in shoulder mechanics.
Identifying the primary location of shoulder pain is helpful in targeting your treatment. For example, pain that is on the more lateral aspect of the shoulder is more indicative of distal supraspinatus or subacromial bursa injury. Pain on the anterior aspect of the shoulder is more likely the result of a distal subscapularis or biceps tendon disorder. Using appropriate assessment strategies helps you narrow down the focus for your treatments so they can have the greatest success.
In other situations, like the serratus anterior weakness we discussed, massage can also be helpful. While the primary problem is muscle weakness, our treatment strategies are not aimed at strengthening the muscle. The serratus anterior is not weak from lack of use. It is weak from compression of a motor nerve.
Therefore, our treatment should focus on trying to relieve pressure on the nerve and restore proper nerve conduction through that motor nerve. Because it is often soft tissues that are compressing the long thoracic nerve, massage applied to the cervical and upper shoulder girdle can have a great impact on reducing the biomechanical dysfunctions associated with serratus anterior weakness.
Become Knowledgeable of Shoulder Pathologies
When you can demonstrate a thorough understanding of key factors such as shoulder mechanics, pathologies and helpful treatment methods, the client is likely to have much greater confidence and perception of likely improvement. For that reason, a solid understanding of anatomy, mechanics, psychological factors, neurophysiology, and other areas all come together to produce the most effective client outcomes.
In addition, treatment strategies that provide comforting touch can decrease noxious input to the sensory system. These neurophysiological effects go a long way to improving the condition and should not be underemphasized.
Several years ago, while at a scientific pain conference, one of the researchers said to me that massage therapy seemed to be one of the most effective means of addressing this comprehensive biopsychosocial picture of so many pain complaints. When we can align our treatment strategies with those outcomes, we get exceptional results for our clients.
About the Author

Whitney Lowe, LMT, directs the Academy of Clinical Massage. He teaches continuing education in advanced clinical massage through the academy and offers an online training program in orthopedic massage. His articles for MASSAGE Magazine include “Make Orthopedic Massage More Effective Using Active Engagement Techniques” and “The Human Body Isn’t a Machine: Structure, Posture & the Role of Assessment in Addressing Pain.”