Last Updated on February 26, 2025 by MASSAGE Magazine
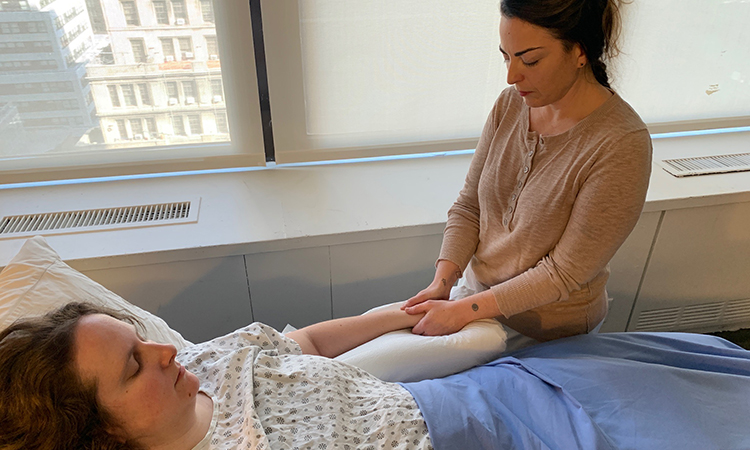
Note from the author: In the month that has passed since the deadline for this article, the landscape in health care has drastically changed due to the spread of the coronavirus / COVID-19. Many massage therapists working in hospital settings have been laid off or asked to perform other tasks for patient care which would normally be considered outside of their scope, as integrative health practices such as massage therapy may be considered non-essential in times of health crises. In the (hopefully near) future when the social distancing parameters are safe to suspend, massage therapists working in integrative settings and elsewhere may expect a positive outlook as clients and health care practitioners are likely to be more acutely aware of the need for touch therapies. Photos by Brogan Wikarek
As a massage therapist and Reiki practitioner, I have found that Reiki and other forms of energy work can be especially meaningful for those clients who are ill, injured or nearing the natural end of their lives.
This article will focus on clients who are in the hospital and discuss how this work can be beneficial in that environment.
Touch is Our Foundation
In human embryos, touch is our first sense to develop. Within two months of conception, the first sensory receptors are formed and continue to develop in utero. Touch, therefore, can be the alpha and omega of human experience. It is our primary connection to others; and in that connection, a reflection of ourselves, our human-ness.
When illness or injury occurs, as is often the case for those in the hospital, a patient may lose their sense of self as the condition, treatments or interventions take over. Clients may feel that their body has turned on them or is failing them. As a reaction to trauma, and at the end of life, there may be a natural dissociation from the body.
Touch can bring pain reduction and relieve anxiety, but it can also help restore a positive sense of self, and a loving image of the body, for clients who are experiencing health difficulties or are transitioning away from life.
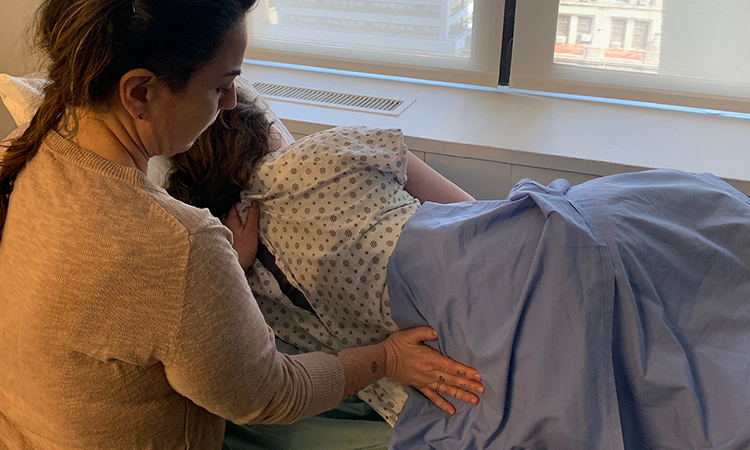
Why Bring Energy Work to the Hospital?
A client may spend extended periods in a hospital setting, on bed rest, with limited mobility, and removed from their loved ones, routines and comfort of home. Massage therapy and energy work can provide a much-needed respite from these difficult situations. These practices do not change the circumstances, but the comfort of touch and connection can call the client into the very present moment, to be here now with their body, instead of living in future “what-ifs?” and past “I should haves.”
When I am preparing interns to work in a hospital setting with clients, it is the be here now approach that I emphasize. As empathetic, compassionate practitioners it is easy to get caught up in the client’s adverse situation, becoming emotionally overwhelmed by the sad story we mentally create about them.
I also advise students to forget most of what they know about massage. Hospital work will be less about movement, tissue manipulations and depth of pressure. It may feel like they are doing nothing, compared to the type of work they have been learning and applying in their clinic settings.
It is this work that reminds us of why we came to the practice of massage in the first place. This work calls us back to the primal sense and power of touch itself. It is less about doing, and more about being with.

Approaches to Energy Work
The word Reiki is made of two Japanese words — Rei, which means “Higher Power” and Ki, which is life force energy. Defined, Reiki is a Japanese technique for relaxation and stress reduction that also promotes healing. It is based on the concept that an invisible life force energy flows through us and causes us to be alive.
In my approach to working with clients in the hospital, I draw on several different modalities; it is important for the therapist to be ready with a range of approaches, including energy work such as Reiki, and other methods such as Comfort Touch, acupressure, reflexology and the Rosen Method.
Comfort Touch, according to its website, is “a style of massage developed by Mary Kathleen Rose, CMT, that gives special consideration to the physical and emotional needs of the elderly and/or ill client.” These principles are outlined as the acronym S.C.R.I.B.E.: Slow, Comforting, Respectful, Into Center, Broad, Encompassing. Each word is a good prompt for the therapist to remember as they work with touch in the hospital setting.
I am also very influenced by Marion Rosen, a physical therapist who worked with psychologists such as Carl Jung. “Rosen Method Bodywork is an experiential body-centered somatic modality that uses a combination of gentle, respectful touch and verbal communication related to the client’s experience and what is felt in the client’s body by the practitioner. The intention within a RMB session is to invite relaxation, self-awareness, and the experience of self-connection.”
The key elements of touch, connection with the breath, and verbal communication can be vital to the therapist and the client during the therapeutic experience. Rosen is a brilliant practitioner, and I encourage students to listen to her videos/recordings to get to an understanding of the approach to this work. She captures the essence of it by saying, “It is not what we do with clients, it is who we are with them.”
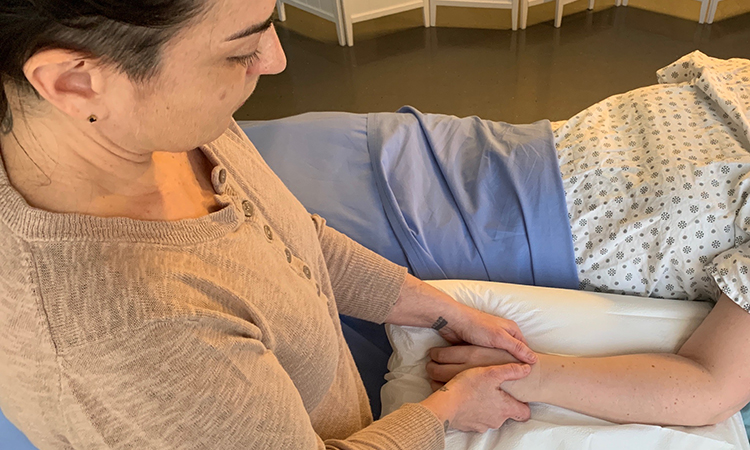
The Hospital Environment
In addition to alterations to the approach to massage or energy work itself, there are other preparations for the therapist and alterations to the treatment to consider in a hospital.
First, there may be requirements for onboarding, whether you are hired by the hospital as an employee, serve as a volunteer, or are hired privately by a family (in the last case, to be diligent, you should research the requirements for an independent contractor in that hospital, as they may vary widely).
Many hospitals require submission of immunization records, including the flu shot; some may allow you to decline the flu shot if you commit to wearing a mask through the entire flu season.

You may be required to do set trainings, usually online, for the Occupational Safety and Health Administration (OSHA), crisis response and HIPAA compliance. The Joint Commission (formally known as, and still referred to by many as JCAHO) is a national hospital accreditation organization, and creates and upholds standards for hospital care. While many hospitals are moving toward integrative care as per JCAHO’s recommendations, there are steps that need to be followed closely in order to be considered in compliance.
You may also be required to show proof of certifications/trainings for the specific population, such as oncology, pediatrics or pregnancy, that you plan on serving in the setting. Even if you are not legally required, ethically, you should be well-prepared with additional training for safety and to provide truly patient-centered care.
Some basics to be aware of:
- You
will need to work around the patient’s schedule of tests, procedures and daily
exams, which can vary from day to day. - You
will be working around equipment — the hospital bed has rails that can be brought
up and down, and the bed itself can be moved up and down and in various level
and reclining positions, but you will need to know how to adjust, and always
leave everything in a safe manner; for example, not leaving the bed far from
the floor, posing a fall risk for the patient when they get up. - You
may be working around local contraindications such as incisions, IV lines or bandages
and will need to make note of these each session, as there may be patient-care changes
even within the same day. - Depending
on the client’s allowances for mobility, you may suggest they move to a chair
in their room or in another setting in the hospital, for a change of scenery or
more privacy, but this will need to be determined with the nurse for safety and
the patient’s schedule.
A Typical Session
Reiki and other energy work can be performed with a direct laying of hands on the body, with hands just hovering over the body, or even from a distance. If the client consents, I prefer to lay hands directly on the body; however, I always give the client a choice, and there are times when the client prefers not to have direct touch.
In either case, during sessions it is important to remain relaxed in one’s own body as the therapist, so that we can maintain our body positions for extended periods without discomfort.
The client can remain fully clothed, even covered with a blanket if they are cold. If your hands are in contact, the depth of pressure is not much more than the weight of the hands themselves.
Sessions may be shorter (15-20 minutes) so as not to overwhelm the client, but longer sessions (45-60 minutes) may also be appropriate depending on the client’s case.
Each client’s response to Reiki may be different, but generally, they report feelings of calm, relaxation, lightness, warmth, connection, care, relief, and “drifting” or “floating.”

Reiki Training
I encourage students to participate in Reiki training and attunement. If they do, they can fully understand the concept of their own Ki and how to give Reiki as a continuous circuit with the client without feeling like it is an energy exchange that puts them at risk of taking on the client’s negative energy; Reiki can actually be quite energizing for the giver.
It is important to note that while there is research to substantiate the efficacy of Reiki, some medical institutions may be opposed to energy work and may be more comfortable with recognizable terms such as massage therapy, or Therapeutic Touch, which is a method developed by nurses. However, it is equally important to give credit where it is due, and be aware of the influence that Reiki and Eastern modalities have had on Western-based approaches.
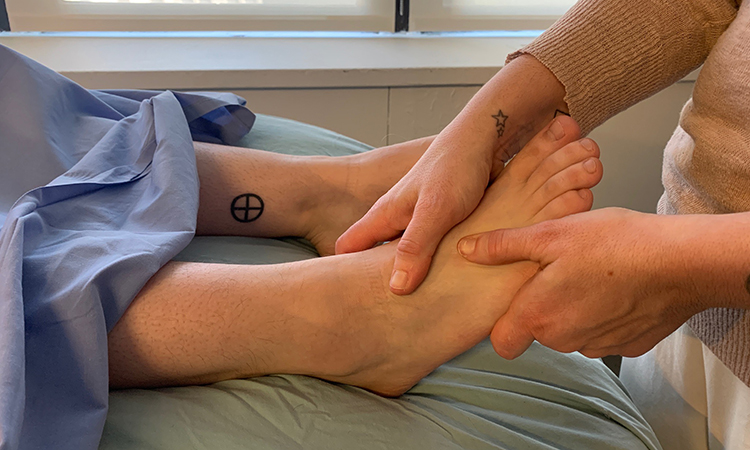
Presence Makes a Difference
Caregivers may have become afraid to touch, viewing their ill relative as fragile. But, the quality of touch may matter less than the touch itself. A 2008 study in Annals of Internal Medicine looked at massage therapy versus simple touch for patients with advanced cancer, and found that massage was more effective on pain and mood, but the control group receiving simple touch also experienced improvements in those areas.
It is pivotal for us to empower clients and caregivers with the reminder that simple touch can also be effective. This allows for sustainability of the benefits beyond our time in the room with them.

About the Author
Kiera Nagle, LMT, CPMT, began practicing massage and Reiki in 2008. As faculty at City University of New York, she is a supervisor at Northwell – Katz Women’s Hospital. She is director of the massage therapy program at Pacific College of Health and Science – NY. Nagle created MaMassage, a CE course for perinatal massage. In conjunction with Womankind, she was the 2018 recipient of a Massage Therapy Foundation Community Service Grant.
References & Further Reading
1. Fagard, J., Esseily, R., Jacquey, L., O’Regan, K., & Somogyi, E. (2018). Fetal Origin of Sensorimotor Behavior. Frontiers in neurorobotics, 12, 23. https://doi.org/10.3389/fnbot.2018.00023
2. Hu, H., Shear, D., Thakkar, R., Thompson-Lastad, A., Pinderhughes, H., Hecht, F. M., & Lown, E. A. (2019). Acupressure and Therapeutic Touch in Childhood Cancer to Promote Subjective and Intersubjective Experiences of Well-being During Curative Treatment. Global advances in health and medicine, 8, 2164956119880143. https://doi.org/10.1177/2164956119880143
3. Smith, M. C., Yamashita, T. E., Bryant, L. L., Hemphill, L., & Kutner, J. S. (2009). Providing massage therapy for people with advanced cancer: what to expect. Journal of alternative and complementary medicine (New York, N.Y.), 15(4), 367–371. https://doi.org/10.1089/acm.2008.0391
4. Vergo, M. T., Pinkson, B. M., Broglio, K., Li, Z., & Tosteson, T. D. (2018). Immediate Symptom Relief After a First Session of Massage Therapy or Reiki in Hospitalized Patients: A 5-Year Clinical Experience from a Rural Academic Medical Center. Journal of alternative and complementary medicine (New York, N.Y.), 24(8), 801–808. https://doi.org/10.1089/acm.2017.0409
5. Armstrong, M., Flemming, K., Kupeli, N., Stone, P., Wilkinson, S., & Candy, B. (2019). Aromatherapy, massage and reflexology: A systematic review and thematic synthesis of the perspectives from people with palliative care needs. Palliative medicine, 33(7), 757–769. https://doi.org/10.1177/0269216319846440
6. Zeng, Yvette S. et al. Complementary and Alternative Medicine in Hospice and Palliative Care: A Systematic Review. Journal of Pain and Symptom Management, Volume 56, Issue 5, 781 – 794.e4
7. Stöckigt B, Suhr R, Sulmann D, Teut M, Brinkhaus B: Implementation of Intentional Touch for Geriatric Patients with Chronic Pain: A Qualitative Pilot Study. Complement Med Res 2019;26:195-205. doi: 10.1159/000496063
8. Schultz, Stacey, MS, MPH. Rosen Method Bodywork at the End of Life Observations from a Massage Therapist. Rosen Method International Journal. Volume 10, Issue 1, 2017. https://1xhdko41sric25njz22ditir-wpengine.netdna-ssl.com/wp-content/uploads/2018/03/RMIJ_vol10_1_Schultz.pdf
9. https://www.reiki.org/faqs/what-reiki
11. https://roseninstitute.net/journal/journal-volumes/
13. https://therapeutictouch.org/
14. Kutner, J. S., Smith, M. C., Corbin, L., Hemphill, L., Benton, K., Mellis, B. K., Beaty, B., Felton, S., Yamashita, T. E., Bryant, L. L., & Fairclough, D. L. (2008). Massage therapy versus simple touch to improve pain and mood in patients with advanced cancer: a randomized trial. Annals of internal medicine, 149(6), 369–379. https://doi.org/10.7326/0003-4819-149-6-200809160-00003