Last Updated on August 19, 2024 by MASSAGE Magazine
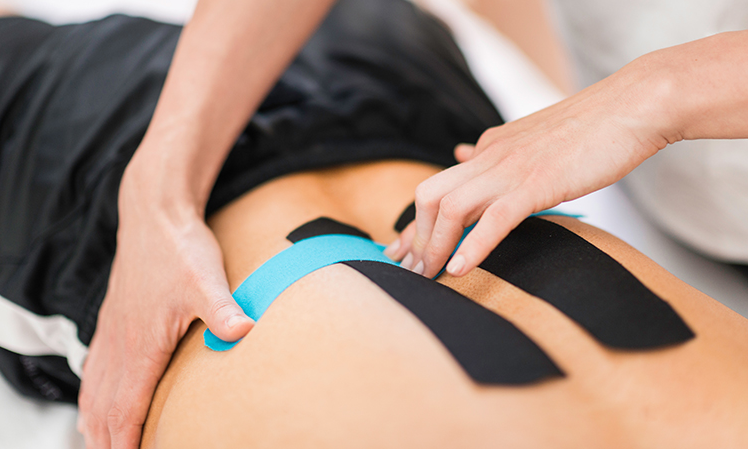
Kinesiology Taping for Massage Therapists explains how kinesiology tape can improve massage therapy by helping with pain, swelling, and muscle tension. Although it was initially underestimated, this tape is now recognized as a useful tool that changes how the brain perceives pain by applying different levels of tension to the skin. Massage therapists can easily add taping to their practice using simple techniques like the anchor and zone methods, which enhance the effects of massage. Whether you’re dealing with a muscle strain, swelling, or a trigger point, kinesiology tape can be a helpful addition to massage sessions.
By now, most massage therapists have seen or heard of kinesiology tape — but how many of us know what it is really doing or at least attempting to do? I was introduced to kinesiology taping in 1995, while working as an athletic trainer.
At the time, kinesiology tape was just arriving on the scene at the National Athletic Trainers Association conference in Portland, Oregon. We all saw it as some fancy elastic tape that was colorful but too flimsy to do the job that athletic tape could do.
Sure, the colors were nice, but the tape provided no stability and was impossible to tear. Kinesiology tape quickly got pushed to the back of the cabinet.
Years later, when I heard sports massage therapist Benny Vaughn, LMT, ATC, discussing the use of kinesiology tape in his practice as an adjunct to his massage work, I re-engaged with the idea of using the tape.
One of the biggest reasons I started to use kinesiology tape in my practice was the fact that it is typically outside our scope of practice to use other common interventions such as ultrasound or e-stim, and I wanted to create a niche in my service offerings that prolonged the outcomes of my work.
Kinesiology tape has been shown to provide similar results as these modalities and is within the scope of most massage therapy practices across the U.S.
Taping Shuts the Gate
Kinesiology taping is a simple way to not only enhance your outcomes, but also to serve as a compliance tool for your clients. Like riding a bike, kinesiology tape can be an easy concept to pick up — but we could all benefit from a little guidance and support in the beginning before we are ready to take off the training wheels and start to ride like a pro.
Kinesiology tape acts as a storyteller. By using varying degrees of tape stretched over and around such target tissues as points of pain, muscles, joints or areas of swelling, we change the afferent messaging being sent to the brain.
As we see more frequently in the biopsychosocial model of pain, as clinical scientist and pain researcher Lorimer Moseley said, “Pain is always, 100% of the time — no exceptions — created by your brain and it makes you do something to protect your body.”
By providing higher degrees of tape tension, we create a mechanical/thermal input. Through lesser degrees of tape tension, we provide a biomechanical lift to the space just below the skin, to assist lymphatic flow. This essentially shuts the gateon the pain experience.
Pain science is one of the most unknown of the sciences. This is primarily due to the brain being the most complex piece of technology in the world. Pain is an output from the brain and not an input from the tissues.
Below is the abstract from research conducted by Canadian psychologist Ronald Melzack, PhD, one of the co-creators of the gate control theory of pain. (“Pain and the neuromatrix in the brain,” Journal of Dental Education, 2001.) He is discussing how pain science has evolved significantly since his and his colleagues’ 1965 findings and why it is imperative that we consider many other factors when addressing an individual’s pain problem, beyond where it hurts:
“The neuromatrix theory of pain proposes that pain is a multidimensional experience produced by characteristic ‘neurosignature’ patterns of nerve impulses generated by a widely distributed neural network — the ‘body-self neuromatrix’ — in the brain.
“These neurosignature patterns may be triggered by sensory inputs, but they may also be generated independently of them. Acute pains evoked by brief noxious inputs have been meticulously investigated by neuroscientists, and their sensory transmission mechanisms are generally well understood. In contrast, chronic pain syndromes, which are often characterized by severe pain associated with little or no discernible injury or pathology, remain a mystery.
“Furthermore, chronic psychological or physical stress is often associated with chronic pain, but the relationship is poorly understood.
“The neuromatrix theory of pain provides a new conceptual framework to examine these problems. It proposes that the output patterns of the body-self neuromatrix activate perceptual, homeostatic and behavioral programs after injury, pathology or chronic stress.
Pain, then, is produced by the output of a widely distributed neural network in the brain rather than directly by sensory input evoked by injury, inflammation or other pathology.
“The neuromatrix, which is genetically determined and modified by sensory experience, is the primary mechanism that generates the neural pattern that produces pain. Its output pattern is determined by multiple influences, of which the somatic sensory input is only a part, that converge on the neuromatrix.”
This means that beyond the sensory input being received, the brain considers many more factors when determining how much pain we really feel; hence, the reason why we all experience pain differently.
These neurosignature patterns may be triggered by sensory inputs from something such as a muscle strain, but they may also be generated independently of them (think chronic pain).
More Studies are Needed
Clinically speaking, I have had consistent success using kinesiology tape for reducing pain, swelling and spasm, as well as improved proprioception and postural awareness. Scientifically, current evidence only supports the use of tape for pain and swelling.
In a systematic review with meta-analysis focused on pain and also methods of tape application, published in the British Journal of Sports Medicine, the authors concluded, “There is benefit to using kinesiology tape in patients with chronic musculoskeletal pain to help reduce pain, even after they leave the clinic.”
This review and other types of research are still not enough for anyone to declare that kinesiology taping does (insert mechanistic outcome); however, we are seeing significant clinical outcomes that should not be ignored.
I am of the mindset that we shouldn’t throw the baby out with the bathwater — meaning just because there isn’t enough evidence to support what we are seeing clinically we shouldn’t discard our clinical outcomes as sham or placebo effects.
We simply need more well-constructed studies, just as we do in massage therapy and so many other fields of health care.
Add Taping to Sessions
Let’s take a look at how you can easily implement kinesiology taping into your daily practice. For starters, we can use just two methods of application, which I call zone and anchor. In the anchor method, the first piece of tape we lay down is your anchor.
In the zone method, the first piece of tape we lay down is over the targeted area referred to as the therapeutic zone. The last part of the tape we lay down with both methods is referred to as the end. Anchors and ends should be 1 to 2 inches long and are always applied with no stretch. This allows the tape to stay on without the risk of it popping off with movement.
Next, focus on these four options: pain, muscle, swelling or joint. These refer to our primary target tissue(s). Each option determines the recommended amount (percentage) of tape stretch to achieve the desired result. These percentages are a result of me and my colleagues gathering lots of scientific and clinical data.
Last, we will always place the target tissue on a stretch prior to laying down our tape, unless our target is a joint, in which case we would not. (Ligaments don’t like to be stretched, do they?)
With any taping application, it is important to note that you always round the corners of the tape. Failure to do this will not impact the objective of the applications but may significantly diminish the wear time of the applications, because the corners can easily be caught by clothing.
Where I see applications fail the most is in this preparation phase. The skin must be cleaned with alcohol, and tape should never be applied over hair. This will eliminate any chance of lift as well as provide channels where moisture can get under the adhesive. Failure to observe these two things will negate any chance of effectiveness.
When applied correctly, tape will typically remain intact for at least five days. It may be worn in the shower or while swimming and just needs to be patted dry upon exiting the water (do not use a blow dryer).
Client Compliance
There may also be a time where you will do multiple types of applications for the same condition. Using the hamstring application as an example, we may determine that along with reducing tone in the muscles, we may also want to apply an additional pain application similar to that done for a trigger point, over the point of pain in the client’s hamstring, further enhancing the amount of sensory messaging to the brain.
Often a client who has been taped will report that they felt like they are taking the therapist’s hands home with them. This also serves as a great client compliance tool, as it provides them with both visual and sensory cues.
Now that we have an overview of how to use the tape, let’s see how we can use it for some common conditions we encounter in our treatment rooms. I encourage you to read this article first and then go back and follow the steps while applying the tape to a friend.
Kinesiology Taping a Myofascial Trigger Point
Type: Pain
Method: Zone
Target: Point of pain
Tension: 50 percent
Objective: Decrease pain
Tape Cut: I-Cut x2
Start by placing the target tissue on a stretch. Measure the piece or pieces of tape, be sure to allow an inch on either end. Break the tape in the middle and peel back the paper, exposing the middle 1/3 of the tape. Place a 50 percent stretch on the tape and lay it down over the point of pain (therapeutic zone). Lay down your ends with zero tension.
Activate the adhesive by rubbing the tape for 20-30 seconds, while the tissue is still on a stretch.
Repeat these steps with a second piece perpendicular to the first piece. This will provide your patients with some additional sensory input to the tissues, reminding the brain that “all is well.”
Watch Drew Freedman demonstrate taping for point of pain, here.
Kinesiology Taping Hamstring Strain
Type: Muscle
Method: Anchor
Target: Biceps femoris, semimembranosus or semitendinosus
Tension: 25 percent
Objective: Reduce tone
Tape Cut: I-cut timestwo
• Start by measuring the target tissue area after it has been placed on a stretch. Failure to do this will result in cutting the tape too short.
• To reduce tone in the hamstring, we will measure our two pieces from both the medial and lateral aspects of the knee, up to the ischial tuberosity.
• Next, break the first I-cut at the end to expose your anchor, the first piece laid down on the skin. Pull the paper backing from the tape until the last couple of inches. Place a 25 percent stretch on the tape and lay it down over the therapeutic zone (Biceps femoris). Lay down your end with no tension. Activate the adhesive.
• Repeat for the medial side of the hamstrings.
Watch Drew Freedman demonstrate taping for hamstring strain, here.
Kinesiology Taping Shoulder Bursitis
Type: Swelling
Method: Anchor
Target: subacromial bursa
Tension: 10 percent
Objective: Reduce swelling
Tape Cut: Fan-cut
• Start by measuring two I-cuts from the proximal attachments of the anterior and posterior deltoid. Next, we will make 6 longitudinal cuts on each piece, allowing 1-2 inches for the anchor. Once the cuts are completed, the tape can be hard to handle, so take the time in preparation to properly break the tape at the base of your anchor, and fold up each paper tendril, exposing the adhesive near the anchor of the tape.
• Lay down your first anchor at the origin of the posterior or anterior deltoid. Laying down one tendril at a time with just 10 percent tape tension, spreading the tendrils in a manner that cover the entire deltoid. Activate the adhesive. Repeat this step with your second piece of tape. Activate the adhesive.
• Make certain that for each piece the anterior/posterior deltoids are placed on a stretch, being mindful of client comfort.
Watch Drew Freedman demonstrate taping for shoulder bursitis, here.
About the Author:

Drew Freedman, BCTMB, CKTSI, is the principal and owner of The Boston Bodyworker and Learn2Tape. He has been a massage therapist for more than 20 years. He received his degree in sports medicine and communications from the University of South Florida, where he also served as an athletic trainer. He received his massage education at Suncoast School of Massage.